By David Cohen, MD, FACC, FHRS,
Cardiology & Cardiac Electrophysiology
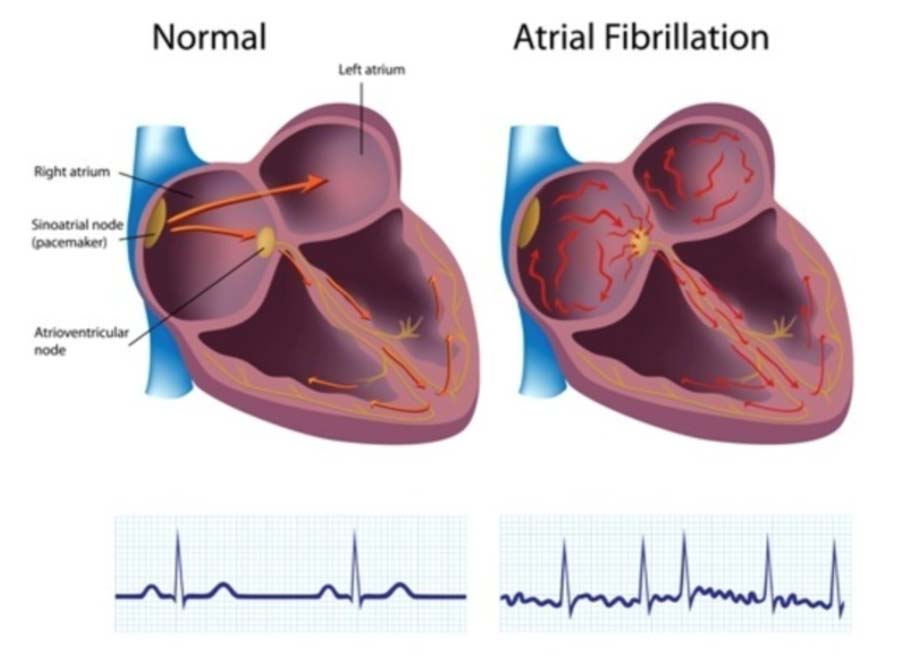
Atrial Fibrillation — also known as AFib or AF — is the most common arrhythmia. It affects more than 2.5 million American adults, and accounts for approximately one-third of hospitalizations for cardiac rhythm disturbances.
It is characterized by a rapid and irregular heartbeat caused when the top chambers of the heart (the atria) quiver (fibrillate) erratically, sometimes faster than 200 times per minute. Afib can have a significant negative impact on an individual’s quality of life, causing heart palpitations, chronic fatigue, higher propensity for heart failure and can increase the risk of stroke up to 5-fold.
Treatment for Atrial Fibrillation
- Reducing the risks of blood clots and stroke with an anticoagulant (blood thinner). The necessity of an anticoagulant depends on a patient’s risk factors, which include hypertension, diabetes, prior stroke, heart failure, and advanced age. In the past Coumadin was the mainstay of anticoagulation, however today novel oral anticoagulants (Eliquis, Xarelto, Pradaxa) have been shown to be safer, more effective and simpler to take.
- Resolving symptoms, either by maintaining normal rhythm in patients with paroxysmal (episodic) Afib or controlling the heart in patients with chronic (permanent) Afib.
a. Medications used to control (i.e. slow) the heart rate during Afib include beta-blockers and calcium channel-blockers, while medications to maintain normal rhythm include a variety of anti-arrhythmic drugs.
b. Restoring normal rhythm in patient with persistent Afib that is either rapid and/or symptomatic involves direct current cardioversion, a simple procedure that involves applying a controlled shock to the chest while the patient is put briefly to sleep.
c. Maintaining normal rhythm long term to avoid the need for chronic medical therapy and/or repeat direct current cardioversions requires a minimally invasive procedure called catheter ablation.
Catheter Ablation for Atrial Fibrillation
Catheter ablation is a minimally invasive procedure performed by an Electrophysiologist in a specialized hospital lab with a team of highly trained nurses and technicians. The Electrophysiologist advances catheters via the large veins in the legs (femoral veins) into the cardiac chambers to target the abnormal electrical signals that trigger and propagate AFib.
These abnormal AFib circuits originate within the pulmonary veins, which are large blood vessels that drain blood from the lungs into the left atrium. Pulmonary vein isolation (PVI) is the standard ablation technique for blocking these abnormal signals from spreading and continuing AF.
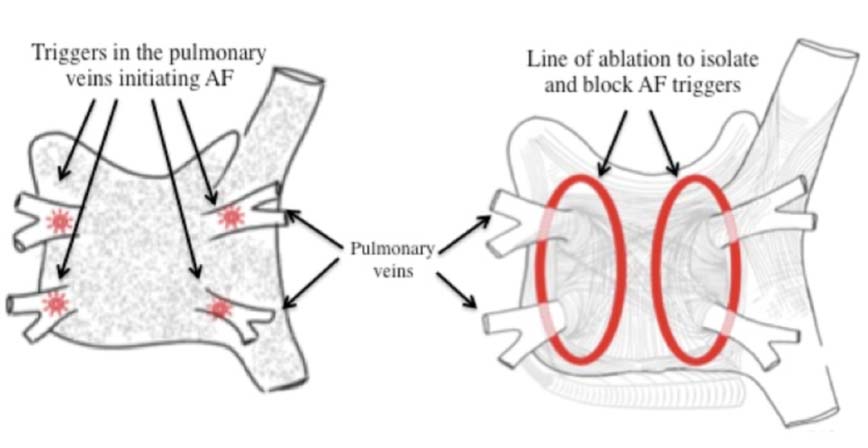
Two main techniques are currently used to perform PVI: traditional radiofrequency (RF) catheter ablation and newer cryoballoon ablation technology. In RF ablation, heat is applied to cauterize tissue whereas in cryoablation, cold energy is applied. In RF ablation the tip of a focal catheter is heated to cauterize tissue in a point-by-point fashion, whereas with cryoballoon ablation a freezing balloon applies continuous cold energy over the larger balloon-tissue surface.
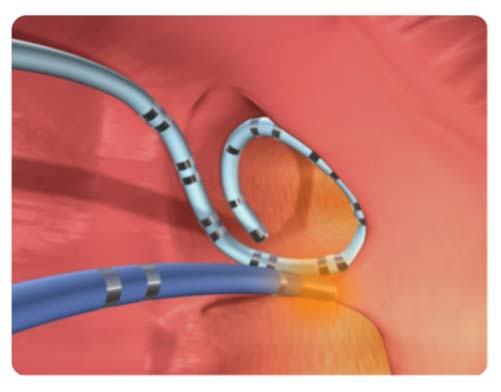
Radiofrequency Catheter Ablation
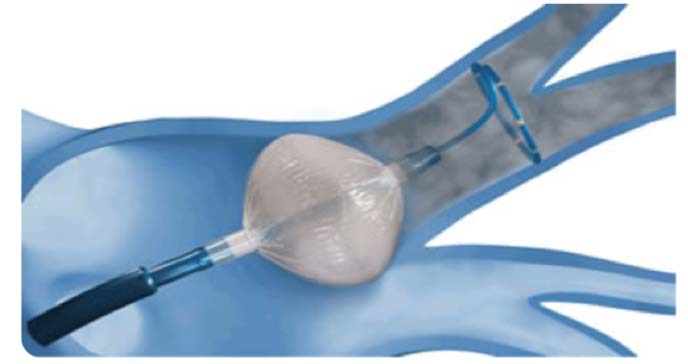
Cryoballoon Ablation
The goal of both types of ablation is to create circumferential scar tissue around the pulmonary veins for their electrical isolation.
The spherical shape of the cryoballoon is designed specifically for pulmonary vein isolation, allowing for safe, efficient, and effective circumferential cryoablation of each pulmonary vein.
- In contrast to point-by-point focal RF ablation, balloon cryoablation creates a continuous line of scar around the pulmonary vein with a single application, allowing for shorter procedural times.
- The compliant surface of the cryoballoon allows for safer manipulation within the thin walled chamber of the left atrium to prevent cardiac injury, in distinction to a stiff, focal RF catheter.
- Cryo-energy is less likely than RF heat energy to cause thermal injury to structures adjacent to the left atrium, specifically the esophagus (the tube that carries food, liquids and saliva from your mouth to the stomach).
The recent FIRE and ICE trial (New England J Med, 2016) found that compared to RF ablation, cryoballoon ablation was equally effective, with statistically significant shorter procedure times, decreased radiation exposure and less serious overall incidence of procedural complications.
 About Dr. Cohen
About Dr. Cohen
Dr. David Cohen underwent intensive training in the cryoballoon ablation technique. He is the leading Electrophysiologist in the San Diego area that routinely performs atrial fibrillation cryoballoon ablation. Tri-City Medical Center is the only hospital in the Northern San Diego Region that provides this cutting-edge technology. Dr. Cohen considers it a privilege and reward to utilize the newest, safest and most effective techniques for patients with atrial fibrillation in the Tri-City community. To learn more about this advanced technology or Dr. Cohen visit Tricitymed.org.