 Osteoarthritis is not only the most common form of arthritis, it is the most common joint disease around affecting more than 10 million people in the United States. It typically manifests in the joints of fingers, thumbs, necks, lower backs, knees, and hips; it is almost most commonly found in people 45 and older and women have a higher rate of prevalence.
Osteoarthritis is not only the most common form of arthritis, it is the most common joint disease around affecting more than 10 million people in the United States. It typically manifests in the joints of fingers, thumbs, necks, lower backs, knees, and hips; it is almost most commonly found in people 45 and older and women have a higher rate of prevalence.
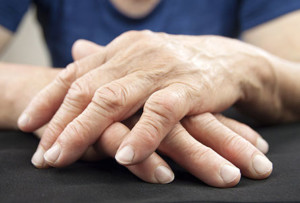
Osteoarthritis affects the joints in one of two ways – it can wear away at the cartilage between joints exposing the ends of your bones to greater wear and tear or it can present itself in the form of painful bumps or spikes called bone spurs. One type in particular, called nodal osteoarthritis, is the culprit of the bony enlargement of joints, particularly in the hands.
The Risk of Osteoarthritis
In addition to age and gender, people who have joints that are not properly aligned are inherently at a higher risk for osteoarthritis. Some of the most recognized misalignments include people with bow legs, dislocated hips, or double-jointedness.
And studies show if a parent or close relative was diagnosed with osteoarthritis, you are at a higher risk for the disease as well due to a hereditary gene defect that can cause deterioration of cartilage in your joints leading to osteoarthritis.
For others, risk sometimes comes at the expense of our experiences, whether we chose them or not. A traumatic joint injury, like the tearing of a ligament or meniscus, can accelerate the onset of osteoarthritis. Or it can be welcomed in through joints that have been overused due to physical labor or sports.
But don’t think that an idle lifestyle is any better for your chances of developing osteoarthritis, because obesity is the next big risk on the list. Being overweight during the middle of your life or your later years is among the strongest risk factors for osteoarthritis of the knee.
Signs of Osteoarthritis
The most apparent signs that osteoarthritis might be on its way include steady or intermittent pain in a joint. Another symptom could be stiffness that tends to follow periods of inactivity, such as sleeping through the night or sitting for an extended period of time. You may also experience swelling or tenderness in one or more of your joints, though that may not necessarily occur on both sides of your body at the same time. And the biggest possibility that you should speak with your doctor is if you experience a “crunching” or “grinding” feeling or hear sounds of bone-on-bone rubbing while you move the problem joint. The official medical term for this sound our sensation is crepitus.
But do keep in mind, osteoarthritis is a disease that takes a relatively long time to manifest in your joints. The gradual condition first begins to develop when your body’s natural bone repair mechanisms of tissue absorption and synthesis get out of balance, allowing bone spurs and bone cysts to grow where they previously didn’t have opportunity to grow. Before they become painfully noticeable, those bone spurs or bone cysts can sometimes be discovered by your doctor through radiographic diagnosis. Common problem areas spotted on an x-ray include an asymmetrical narrowing of joint spaces, a narrowing of the area surrounding a joint (periarticular sclerosis), bone spurs (osteophytes), and a fluid-filled sac of thickened joint lubricant that extrudes from the bone (sub-chondral bone cysts).
How Do I Treat Osteoarthritis?
Once diagnosed, there aren’t too many options available to a patient. That’s because osteoarthritis is a condition that progresses slowly over a period of many years and cannot be cured. The treatments we focus on primarily deal with decreasing the unwelcome symptoms and slowing the continued progress of the condition.
The most successful forms of treatment are the ones that help limit your joint pain, increase the range of motion in your arms and legs, and increase your muscle strength so you can keep doing the things you love to do and prevent falls or other costly injuries.
Depending on your particular circumstances, such treatments can take the shape of non-operative procedures as simple as pain medications, physical therapy, and walking aids, or as complex as shock absorption and re-alignment of joints through special shoes or foot gear (orthotics) that serve to limit strain from bodily weight and movement on the most sensitive joint areas.





